Medical Disclaimer: This article provides educational information about women's sleep health. Always consult with healthcare professionals for proper diagnosis and treatment of medical conditions.
Understanding Women's Unique Sleep Challenges
Women face distinct sleep challenges throughout their lives due to hormonal fluctuations, biological differences, and societal factors. Research from the National Sleep Foundation shows that women are 40% more likely to experience insomnia than men, and hormonal changes during menstruation, pregnancy, and menopause significantly impact sleep quality and duration.
Understanding these gender-specific factors is crucial for developing effective sleep strategies that address the root causes of sleep disruption rather than just treating symptoms. Women's sleep needs and patterns differ from men's in measurable ways that require targeted approaches.
Key Statistic: Studies show that 63% of women report sleep disturbances during their menstrual cycle, with the greatest disruption occurring in the days leading up to menstruation when progesterone levels drop dramatically.
Hormonal Influences on Women's Sleep
Hormones play a central role in regulating sleep-wake cycles, and the cyclical nature of women's hormones creates unique challenges and opportunities for sleep optimization.
Estrogen and Sleep Quality
- Sleep Promotion: Estrogen helps maintain REM sleep and reduces sleep fragmentation
- Temperature Regulation: Higher estrogen levels support better temperature control during sleep
- Mood Stabilization: Estrogen influences serotonin production, affecting sleep quality
- Decline Effects: Estrogen drops during menopause lead to hot flashes and sleep disruption
Progesterone's Sleep Benefits
- Natural Sedative: Progesterone has calming, sleep-promoting properties
- Deep Sleep Enhancement: Higher progesterone levels increase slow-wave sleep
- Anxiety Reduction: Progesterone helps reduce anxiety that can interfere with sleep
- Cyclical Changes: Progesterone fluctuations during menstrual cycles affect sleep patterns

Sleep Strategies for Different Life Stages
Reproductive Years and Menstrual Cycle
The menstrual cycle creates predictable patterns of sleep quality that women can anticipate and manage proactively.
Follicular Phase (Days 1-14)
- Generally better sleep quality as estrogen rises
- Optimal time for establishing new sleep habits
- Take advantage of natural energy for morning exercise
- Focus on consistent sleep schedule during this phase
Luteal Phase (Days 15-28)
- Potential sleep disruption as progesterone drops
- May experience increased sleep need (8-9 hours)
- Practice extra stress management techniques
- Consider magnesium supplementation for PMS symptoms
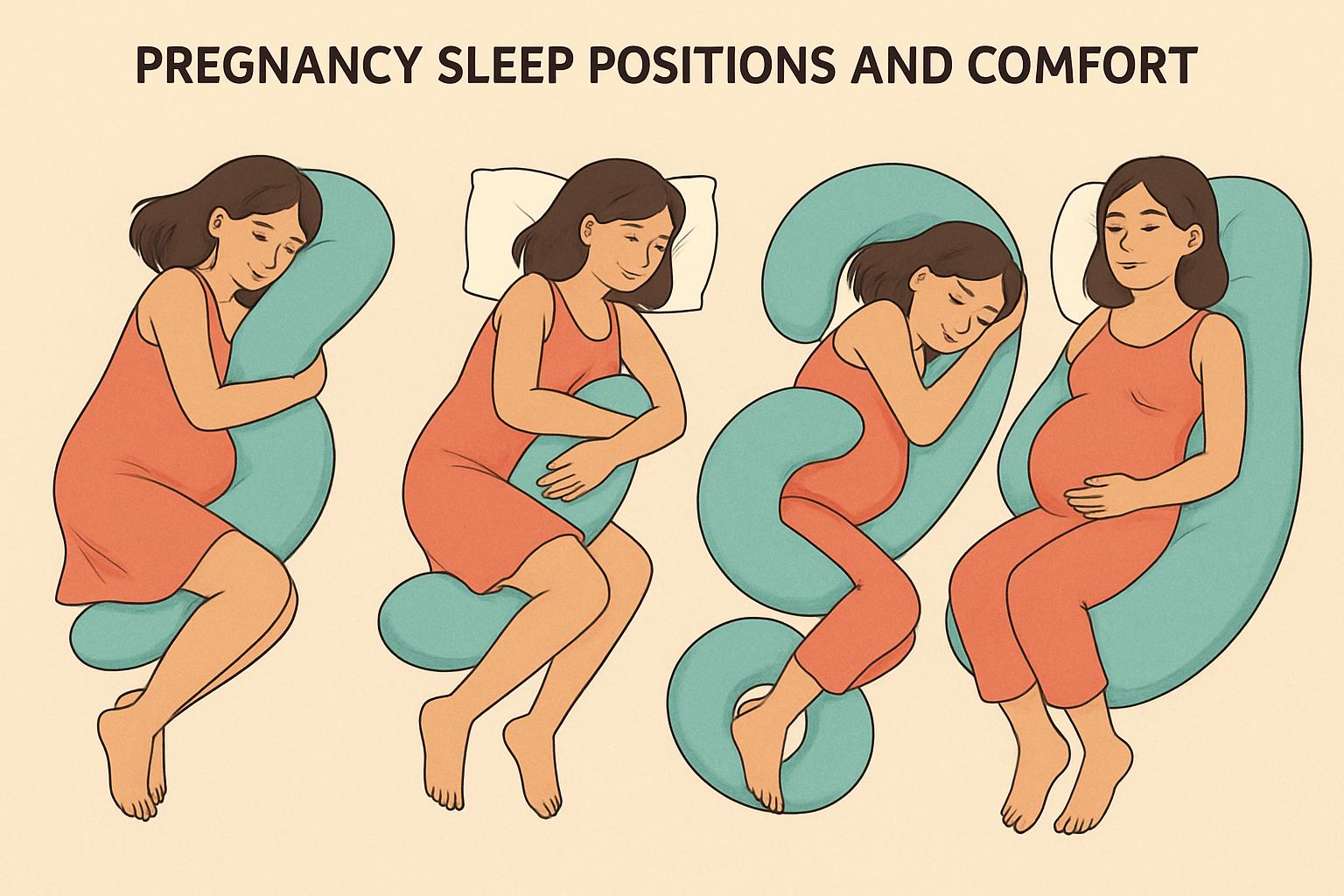
Pregnancy Sleep Optimization
Pregnancy brings unique sleep challenges that change with each trimester, requiring adaptive strategies.
First Trimester
- Increased Fatigue: Allow for 9-10 hours of sleep and short naps
- Frequent Urination: Reduce fluid intake 2 hours before bed
- Nausea Management: Keep crackers bedside for morning sickness
- Hormone Adjustment: Be patient with sleep pattern changes
Second Trimester
- Optimal Sleep Period: Take advantage of improved energy and comfort
- Sleep Position: Begin transitioning to side sleeping (left side preferred)
- Exercise Benefits: Regular prenatal exercise improves sleep quality
- Stress Management: Practice relaxation techniques for better sleep
Third Trimester
- Support Systems: Use pregnancy pillows for comfort
- Heartburn Prevention: Elevate head of bed, avoid late meals
- Frequent Wakings: Practice sleep hygiene for easier return to sleep
- Preparation: Establish postpartum sleep strategies
Pregnancy Sleep Tip: The "SOS" position (Sleep On Side) with a pillow between knees and under the belly provides optimal comfort and blood flow. Left side sleeping is preferred to maximize blood flow to the placenta.
Postpartum Sleep Recovery
The postpartum period presents unique sleep challenges due to newborn care demands, hormonal changes, and physical recovery.
Immediate Postpartum (0-6 weeks)
- Sleep When Baby Sleeps: Prioritize rest over household tasks
- Night Feeding Strategy: Keep lights dim during night feedings
- Support Network: Accept help with night duties when possible
- Recovery Focus: Prioritize healing and adjustment over perfect sleep
Extended Postpartum (6 weeks - 1 year)
- Gradual Schedule: Slowly establish consistent bedtime routines
- Partner Coordination: Share night duties to maximize sleep blocks
- Nap Strategy: Strategic 20-30 minute naps when possible
- Sleep Debt Management: Gradually recover from accumulated sleep debt
Menopause and Sleep: Managing the Transition
Menopause brings significant sleep challenges due to hormonal changes, but understanding these changes enables effective management strategies.
Perimenopause Sleep Changes
- Hot Flashes: Occur in 75% of women, often disrupting sleep
- Night Sweats: Can cause multiple awakenings and discomfort
- Mood Changes: Increased anxiety and depression affect sleep quality
- Sleep Architecture: Reduced deep sleep and increased sleep fragmentation
Menopause Sleep Optimization Strategies
Temperature Management
- Keep bedroom temperature 2-3 degrees cooler than usual
- Use moisture-wicking sleepwear and bedding
- Consider a cooling mattress pad or pillow
- Layer bedding for easy temperature adjustment
Hormonal Support
- Hormone Therapy: Discuss options with healthcare provider
- Natural Alternatives: Consider black cohosh, red clover, or soy isoflavones
- Lifestyle Factors: Regular exercise and stress management support hormone balance
- Timing Considerations: Work with healthcare providers on optimal timing
Sleep Environment Optimization
- Invest in high-quality, breathable bedding
- Use a fan or white noise machine for temperature and sound control
- Consider separate bedding from partner to minimize disturbance
- Keep water and towel bedside for night sweats
Nutrition and Supplements for Women's Sleep
Targeted nutrition strategies can help address women's specific sleep challenges throughout different life stages.
Key Nutrients for Women's Sleep
- Magnesium: 200-400mg before bed helps with muscle relaxation and PMS symptoms
- Iron: Address deficiency that's common in menstruating women and affects sleep
- Vitamin D: Support mood and sleep regulation, especially important during darker months
- B-Complex: Support nervous system function and stress management
- Omega-3 Fatty Acids: Reduce inflammation and support mood stability
Herbal Support Options
- Valerian Root: Natural sedative properties for occasional sleep issues
- Chamomile: Gentle relaxation support, safe during pregnancy
- Passionflower: Helps with anxiety-related sleep problems
- Lemon Balm: Calming properties and stress reduction
Important Note: Always consult with healthcare providers before starting any supplements, especially during pregnancy, breastfeeding, or when taking medications. Individual needs vary significantly.
Stress Management and Mental Health
Women face unique stressors that can significantly impact sleep quality, including caregiving responsibilities, work-life balance challenges, and societal pressures.
Stress-Reduction Techniques
- Mindfulness Meditation: 10-20 minutes daily to reduce cortisol levels
- Progressive Muscle Relaxation: Systematic tension release for physical relaxation
- Journaling: Process daily stressors and clear mental clutter before bed
- Boundary Setting: Establish clear work-life boundaries to protect sleep time
Mental Health Considerations
- Depression Screening: Women are twice as likely to experience depression
- Anxiety Management: Address anxiety that commonly disrupts women's sleep
- Professional Support: Seek therapy for persistent sleep-affecting mental health issues
- Medication Review: Evaluate sleep effects of mental health medications
Creating a Women-Focused Sleep Plan
Developing a personalized sleep strategy that accounts for hormonal changes, life stage, and individual factors is key to long-term sleep success.
Assessment Areas
- Menstrual Cycle Tracking: Identify patterns in sleep quality throughout the month
- Life Stage Considerations: Adapt strategies for current reproductive status
- Stress Evaluation: Assess major stressors and their impact on sleep
- Health Conditions: Consider thyroid function, iron levels, and other health factors
Implementation Strategy
- Start with one area of focus rather than trying to change everything at once
- Track sleep patterns for 2-4 weeks to identify trends
- Adjust strategies based on menstrual cycle phases
- Work with healthcare providers for hormonal or medical concerns
- Be patient with the process - hormonal sleep improvements take time
Success Strategy: Remember that women's sleep needs change throughout life. What works in your 20s may need adjustment in your 40s. Stay flexible and adapt your sleep strategies as your body and life circumstances change.